For many people springtime feels like the end of a long winter, with more daylight and above zero temperatures in southern Finland indicating that summer is on the way. But statistics show that this transition period, from a long, cold, dark winter to the bright light and warmth of summer temperatures, is a high risk period for suicide and suicide attempts. How could this be?
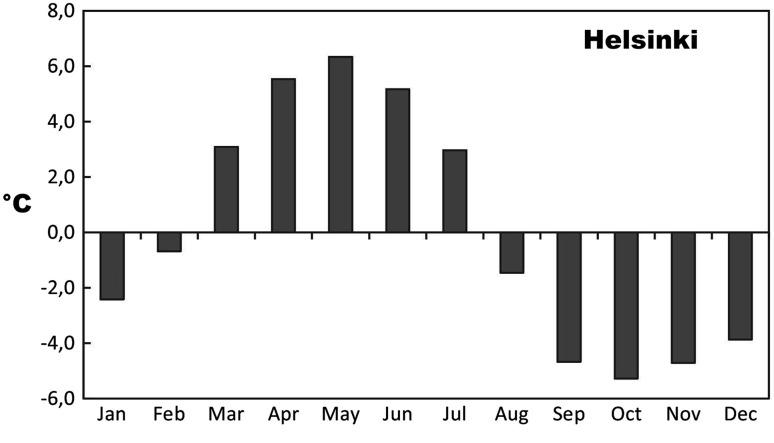
There are a number of theories why this is the case. Some research argues that it is a biochemical reaction in the body due to brown adipose fat tissue being affected by light and causing depression when the temperature is not yet warm (which is the case in the long, sunny but still cold days of spring in Finland). The researchers looked at data from over 160 years of suicide statistics in Finland and found that the peaks of suicide rates are in May (when the temperature increases) and October (when it decreases). They theorise that suicides are related to rapid changes in temperature that affect the body and cause depression symptoms to worsen. In Finland there can be temperature changes of 6 degrees from one month to another in May and October:
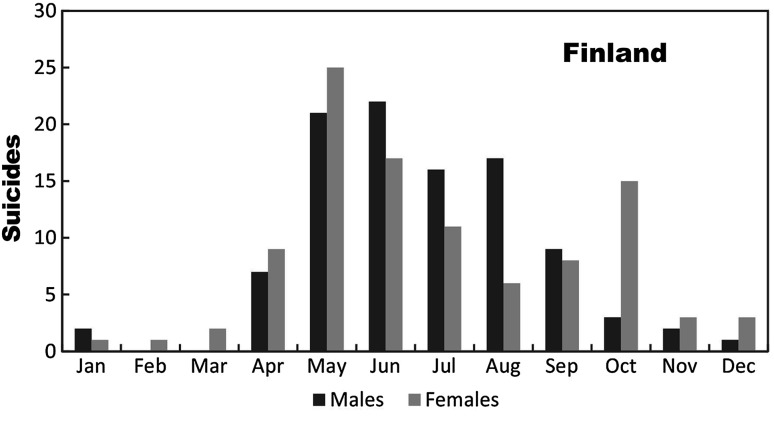
In fact, most suicides in Finland happen in early summer. This seems counter-intuitive – one would think that winter would have higher rates of suicide because it is so dark and depressing. But in fact the data consistently shows that late spring and early summer is the highest risk period.
As a psychologist I would argue that the increase in suicide and suicidal behaviour in spring is also due to the huge difference between our internal state of mind and the external world. In a long Finnish winter depression does not seem to be out of place with the environment. The lack of energy, fatigue, hopelessness and feelings of sadness that accompany depression seem to fit in well with the winter conditions. But when spring arrives and Finland is bathed in near constant light and a summertime atmosphere, the internal world and external world are in conflict. Added to this, other people are active, excited and happy to be enjoying summer, which is quite the opposite of how a depressed person feels. This discrepancy can increase the feelings of loneliness, isolation and helplessness that a person with depression feels, thus increasing depressive symptoms and suicide risk.
Knowing all of this, it is important to be aware of oneself and others, especially men (who account for 75% of suicides in Finland) being at increased risk for suicide in May, June and July.
If you or someone you care about is showing signs of suicide – either acting strangely calm after being depressed for a long time (a signal they have made a decision to make a suicide attempt) or simply telling you about their depression and suicidal feelings – you can take action in a number of ways:
- Suicide is a medical emergency – call 112 or go to a hospital
- In a crisis call the Mieli SOS Crisis helpline in English and Arabic: 09 2525 0113 (Mondays and Tuesdays 11 am-3 pm, Wednesdays 1 pm-4 pm and 5 pm-9 pm, Thursdays 10 am-3 pm) or 24 hrs a day (in Finnish) +358 9 2525 0111
- Seek help from a doctor or your local health station
- Make an appointment with a psychologist at Compass Psychologist or another private practice
If help is not immediately available the person with suicide should be monitored and observed by another person until they are safe. For more information check out this page on free services and where to go in an emergency: https://mentalhealth.fi/where-to-go-in-an-emergency
Suicide should be prevented and a person who is suicidal should get help, but they need help and connection with others. Psychological treatment of suicide usually involves care and compassion from a warm and encouraging health professional or therapist and treatment of the underlying depression. Treatment of depression can involve medication such as anti-depressants, therapy or a combination of the two.
For those relatives and friends of a suicidal person, there is help for you as well, in the form of support organisations such as FinFami (https://finfami.fi/in-english/), or individual therapy for you.

